Biochemists Create Microbicidal Coating to Fight Hospital Infections
New bandages with microbicidal coating kill the most harmful bacteria on contact. The coating is washable and can also be used on hospital gowns and bed sheets, which will help reduce the risk of infection to all hospital patients and staff. Hospital infections are growing to epidemic proportions because they're passed from person to person. Now, researchers are working to wipe out these infections with a new bacteria-killing bandage.
Gary Smithson was hit head-on by a drunk driver. The accident put him in a wheelchair, but that is not what keeps him there. It's what happened in the ER -- hours after the crash -- that has made the past 10 years unbearable. During a routine check, doctors found an infection.
Gary is one of 20,000 Americans that leave the hospital each year with an infection they didn't come in with. Gregory Schultz, a biochemist at the University of Florida in Gainesville, is part of a team working to wipe out these super bugs. They've created a microbicidal coating that can kill the most harmful bacteria.
"The microbicidal agent -- that's the thing that kills the bacteria -- is permanently bonded on the surface of the fibers of the dressing," Schultz says.
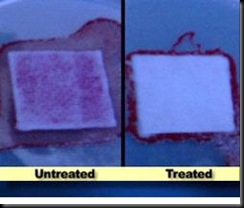
The bandage on the left is not treated with the microbicidal coating. The area in red is infected with bacteria. Now, look at the bandage on the right. It is treated -- you can see there are no bacteria.
Chris Batich, a biomaterials expert at the University of Florida, says, "What we wound up with is a surface that you can wash. And whenever it touches bacteria, it kills the bacteria ... and keeps on killing them."
The microbicidal coating can also be used on hospital gowns and bed sheets, which will help reduce the risk of infection to all hospital patients and staff.
Because of his infection, Gary believes he will spend the rest of his life in wheelchairs he fixes in his shop. "It's completely changed the way I have to live," he says. Every day is a struggle against an invisible invader that Gary hopes won't claim any more innocent victims.
The bacteria-fighting agent can be used outside the hospital for soldiers in the field to help stop athletes foot. The cost of putting this agent on a bandage is about one cent.
BACKGROUND: University of Florida researchers have led the development of a new type of wound dressing that could keep dangerous antibiotic-resistant bacteria from spreading in hospitals, a problem that leads to thousands of deaths in the U.S. annually. Each year, nearly two million Americans contract infections while hospitalized.
HOW IT WORKS: The new wound dressing features a microbial coating that can be chemically bonded to gauze bandages, socks and even hospital bedding and gowns. This makes the material super-absorbent and pulls excess moisture away from the wound. The microbial coating blocks bacteria from reaching a wound and recolonizing there. It also kills the most common and harmful types of resistant bacteria that cause 70 percent of infections in hospitals, such as staph infections. The fabric can be made into clothing, such as antifungal socks and underwear that could help U.S. soldiers in the field who often don't have time to change or shower. Furthermore, the structure of the coating, and the complexity of the process, makes it nearly impossible for bacteria to become resistant to it. Other dressings use a process that allows molecules to diffuse into the air and into the wound, which can slow healing and increases the chance germs will develop resistance.
WHAT ARE STAPH INFECTIONS?
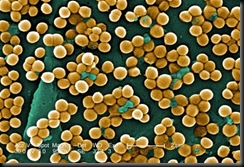 Staph infections result when a bacteria called Staphylococcus aureus enters the body through an open cut or break in the skin. They usually produce pus. Minor staph infections include infections of hair follicles after shaving, or sties, which occur when the follicle surrounding the eyelashes causes a sore red bump in the eyelid. Staph infection is also behind most cases of food poisoning and can also lead to more life-threatening conditions, such as toxic shock syndrome, pneumonia, and infections of the heart of blood. Those in hospitals, with weakened immune systems, are especially vulnerable to staph infection.
Staph infections result when a bacteria called Staphylococcus aureus enters the body through an open cut or break in the skin. They usually produce pus. Minor staph infections include infections of hair follicles after shaving, or sties, which occur when the follicle surrounding the eyelashes causes a sore red bump in the eyelid. Staph infection is also behind most cases of food poisoning and can also lead to more life-threatening conditions, such as toxic shock syndrome, pneumonia, and infections of the heart of blood. Those in hospitals, with weakened immune systems, are especially vulnerable to staph infection.
HOW WOUNDS HEAL: Controlling moisture and staving off infection are two of the most important aspects of wound healing. All wounds go through the same basic stages of healing. A cavity wound is when a large chunk of tissue has been removed, leaving a hole. Small cavity wounds can be closed with stitches, but larger cavities are more prone to infection and are left open to heal. In open healing, the wound "fills in" from the bottom by building new tissue. As it fills in, the sides of the wound also get new tissue. The sides must be kept from touching until the wound has filled in at least halfway, otherwise they can form bridges, trapping fluids in the wound. A healing wound should look bright red. In the active healing phase, cells multiply, connective tissue cells form collagen, and eventually small red fleshy masses of tissue begin to form. These masses keep growing and contracting until the cavity fills up completely.
Source: ScienceDaily

No comments:
Post a Comment